Diagnostic decisions: what is spirometry and why is it important?
Posted on January 09, 2020 |
This post was authored by Barbara Yawn, MD, MSc, FAAFP of the University of Minnesota; M. Bradley Drummond, MD of the University of North Carolina at Chapel Hill School of Medicine; and Carol Rubin, MEd, MS of Cliffside Park, NJ.
What is spirometry?
Spirometry is a common breathing test that assesses how well your lungs work. The test measures how quickly and how much air you can breathe in and out.1 It is part of the testing done with full pulmonary function testing which may include other assessments (see below). During normal breathing, air flows in and out of your lungs freely. However, people with chronic obstructive pulmonary disease (COPD) have a hard time breathing out, and therefore too much air stays in their lungs.2 This is known as “air trapping” and is one of the causes of feeling short of breath.2 Spirometry is an important test that should be done in addition to asking about your symptoms and medical history when COPD is diagnosed.2 Spirometry can help decide what medicines you will take and it can be used to follow your lung health over time.2
What happens during spirometry?
On the day of your test, your doctor may ask that you do not take your COPD medicine, do not wear tight clothing, and do not eat a large meal for two to four hours before your test. When you arrive, a person in your doctor’s office will explain the test and what you need to do. The test takes about 30 to 45 minutes to complete.1 Here is what to expect during your spirometry test1,3:
- You will be seated upright in a chair, and a clip will be placed on your nose to keep you from breathing through your nose.
- With a mouthpiece connected to the spirometer, you will be asked to take a deep breath in, so that your lungs are completely filled with air, and then to breathe out as hard and fast as you can for six to eight seconds—until your lungs are emptied as much as possible.
- You will be asked to repeat these steps at least three times to make sure that the test result is right.
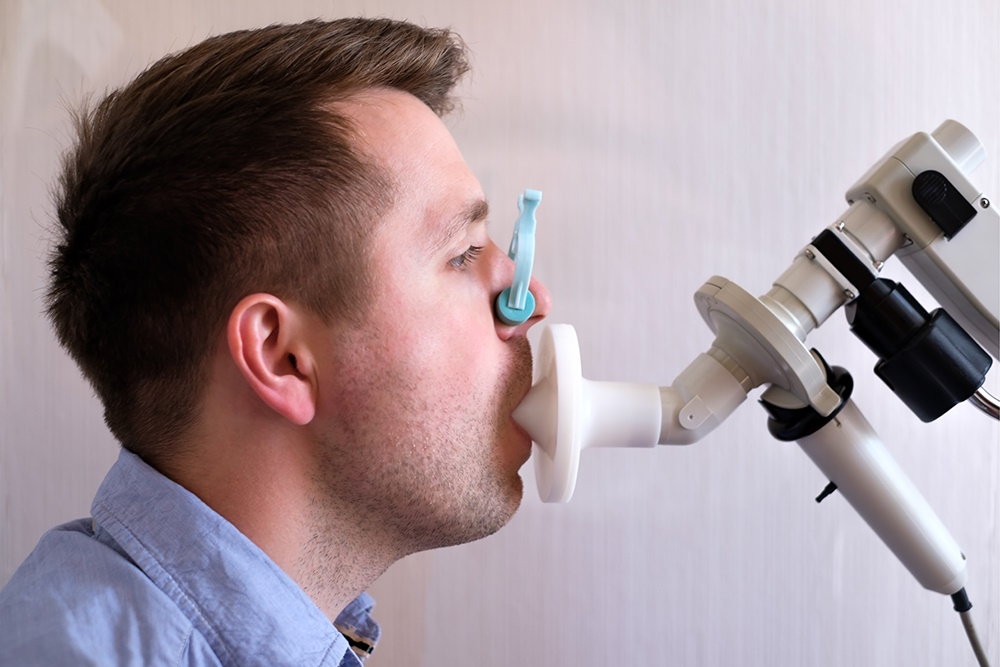
Figure. A person with COPD undergoing a spirometry test
After the first set of tests, you may be given an inhaled medicine, a bronchodilator, to open up your lungs.3 After waiting for about 10 to 15 minutes for the medicine to work, the test is done again. This will help your doctor find out if the bronchodilator improves the air movement through your lungs.
Spirometry should be done if your doctor thinks you may have COPD or if you keep having trouble breathing. You should ask for a spirometry test if you do not have a COPD diagnosis but are often short of breath, if your breathing problems keep you from doing things you would like, or if you have been diagnosed with COPD but your medicines do not seem to be helping.2 Your doctor may also give you a spirometry test if you have noticed a change in your symptoms (See What does it mean when COPD symptoms are “controlled”? Part 1 and Part 2 for more information). Always talk to your doctor before taking a spirometry test. Watch this video to understand how a spirometry test is performed – Taking a spirometry test
How is the spirometry test used?
The spirometry test looks at three important things about how your lungs work2:
- Forced expiratory volume in 1 second (FEV1): The amount of air you can blow out hard and fast in one second after taking a deep breath.
- Forced vital capacity (FVC): The amount of air you can blow out until you empty your lungs after taking a deep breath in.
- Ratio of FEV1/FVC: This is the FEV1 divided by the FVC. This number is used to find out if you have COPD. Those who cannot blow out 70% (about three quarters) of the air in their lungs in the first second have reduced lung function that suggests COPD.
The spirometry test results can vary by a person’s sex, age, race, and height. Your doctor will compare your spirometry test results with those from healthy people. This tells your doctor how your test results compare with someone of the same sex, age, race, and height and is presented as “percent predicted.” If your FEV1 is less than 80% of predicted, it means that your lungs are not working as well as would be expected for someone of your sex, age, race, and height.2
The findings of the spirometry test can be used in the following ways2:
- To find out whether or not you have COPD: If your FEV1/FVC ratio is less than 0.7, you likely have COPD. Spirometry can detect COPD even if you do not yet have symptoms.
- To find out how severe the problems with your lungs are: A low FEV1 suggests that your lungs are “obstructed,” making it difficult to breathe out. Depending on your FEV1 (percent predicted), the level of your COPD may be called mild, moderate, severe, or very severe. This level of COPD can also be used to help choose your therapy and check how your lungs change over time, perhaps after a recent exacerbation or flare-up.
- To find out whether your COPD treatment is helping: Having further spirometry tests once you have been taking your COPD medicines for some time will help your doctor decide if your medicines are helping your symptoms and your lungs, or if you may need more or different inhalers or medicines or pulmonary rehab (rehabilitation).
Your doctor may ask you to have more lung tests called full pulmonary function tests (or PFTs) to learn more about your breathing problems and fully understand your COPD symptoms. These tests measure other things about your lungs, such as the amount of air left in your lungs when you think you have emptied them, and the ability of your lungs to move gases, such as oxygen and carbon dioxide, back and forth from the lungs to the blood stream (called diffusion capacity). This extra information may help you and your doctor decide if other tests are needed or whether other medicines or treatments for your COPD will help.4
Acknowledgments
The authors meet the criteria for authorship recommended by the International Committee of Medical Journal Editors. The authors received no direct compensation for the development of this manuscript. Writing, editorial support, and formatting assistance was provided by Praveen Kaul, PhD, and Frances Gambling, B.A. (Hons), of Cactus Communications, which was contracted and compensated by Boehringer Ingelheim Pharmaceuticals, Inc. (BIPI) for these services. BIPI was given the opportunity to review the manuscript for medical and scientific accuracy as well as intellectual property considerations.
Disclosures
Dr. Yawn reports personal fees from Boehringer Ingelheim, AstraZeneca, GlaxoSmithKline, and Midmark and grants from the COPD Foundation, Boehringer Ingelheim, and the National Heart, Lung, and Blood Institute (NHLBI) outside the submitted work.
Dr. Drummond reports grants from the NHLBI, the U.S. Department of Defense, and Boehringer Ingelheim outside the submitted work. He also reports personal fees from Boehringer Ingelheim, GlaxoSmithKline, AstraZeneca, Mylan-Theravance, Novavax, Parion, Midmark, and Philips outside the submitted work.
Ms. Rubin reports personal fees from Novartis and the U.S. Department of Defense outside the submitted work. She is associated with the COPD Foundation as a State Captain, which is a nonpaid position.
References
- American Lung Association. Spirometry. 2018. Retrieved from https://www.lung.org/lung-health-diseases/lung-procedures-and-tests/spirometry. Accessed: November 20, 2019.
- Global Initiative for Chronic Obstructive Lung Disease (GOLD). Global strategy for the diagnosis, management, and prevention of chronic obstructive pulmonary disease. 2020 Report. Retrieved from https://goldcopd.org/ Accessed: November 20, 2019.
- American Thoracic Society. Pulmonary function tests. Am J Respir Crit Care Med. 2014; 189:P17-P18.
- Ranu H, Wilde M, Madden B. Pulmonary function tests. Ulster Med J. 2011; 80:84-90.