I Have COPD, Now What?
Posted on June 17, 2021 |
This article was written by Angie Brunkhardt, RRT.
So, you have COPD. These words scare even the strongest people. What does having COPD mean? How does your doctor know this is truly the problem? How will COPD affect your life, your future? You probably have a few questions. Let us start by talking about what to expect when it comes to testing.
There is only one diagnostic test that can really confirm if you have COPD. That test is called a pulmonary function test (PFT). One part of the PFT is called a spirometry test. When you schedule your PFT, the testing center will remind you not to take your respiratory medications the day of your test.
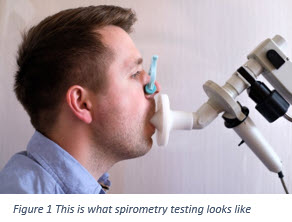 For this test, a respiratory therapist will guide you through a series of breathing/blowing exercises while you have a nose clip and your mouth on a large mouthpiece connected to a spirometer to measure air flow. You will take in very deep breaths through the mouthpiece and blow out very hard and fast for several seconds. You will feel that you are really pushing yourself, and that is exactly the kind of effort needed for this test. You will repeat this test several times to make sure the results are as accurate as possible. When you finish the first part of the test, the respiratory therapist will give you a bronchodilator either by using inhaler or nebulizer, and you will repeat the breathing test again. By repeating the test after using the medication, the doctor can determine if your lung disease reacts to the medication. A positive reaction will show an increase in your numbers and less difficulty with the breathing test exercises you repeat.
For this test, a respiratory therapist will guide you through a series of breathing/blowing exercises while you have a nose clip and your mouth on a large mouthpiece connected to a spirometer to measure air flow. You will take in very deep breaths through the mouthpiece and blow out very hard and fast for several seconds. You will feel that you are really pushing yourself, and that is exactly the kind of effort needed for this test. You will repeat this test several times to make sure the results are as accurate as possible. When you finish the first part of the test, the respiratory therapist will give you a bronchodilator either by using inhaler or nebulizer, and you will repeat the breathing test again. By repeating the test after using the medication, the doctor can determine if your lung disease reacts to the medication. A positive reaction will show an increase in your numbers and less difficulty with the breathing test exercises you repeat.
The next test I would like to talk about is called the six-minute walk test. This test may sound intimidating due to your shortness of breath, but it is important to find out about your exercise endurance and if you have problems with your oxygen. During this test, you will walk as far as you can for six minutes. If, during the test you need to stop and rest, you can do so. The time will keep counting, but the point of the test is to see how much ground you can cover in six minutes. You may perform this test prior to starting pulmonary rehab or your doctor may have you repeat this test periodically to see how well you are maintaining your ability to walk and exercise.
The six-minute walk test is different from the walk test you might do to determine whether or not you need supplemental oxygen. Lack of oxygen can cause a many different medical issues, from heart conditions to memory problems. For this test, you will walk with the respiratory therapist who will be monitoring your oxygen levels with a pulse oximeter clipped to your finger. You will walk for a certain period of time or a certain distance, or until you show difficulty with the test. They will stop the test if you have any issues and rest you before starting again. If your oxygen levels fall below 88, they will let the doctor know that you need supplemental oxygen. When you meet the doctor, ask about all of your options for home oxygen. Not all oxygen providers have the same devices. Certain types of oxygen delivery systems could increase your out-of-pocket price or limit you to the device the company carries only.
 If you are ever in the hospital with breathing problems, or if your doctor thinks it is necessary as an outpatient, he/she might order a test called an arterial blood gas (ABG). This is blood test that requires the respiratory therapist to draw a small amount of blood from an artery instead of a vein like you might be familiar with. Usually, the blood sample is taken from the artery in your wrist right where you feel your pulse in thumb side of your wrist. The location can be very sensitive, so you may feel anxious before the procedure. The best practice would be for you to focus on breathing slowly in and out as they get the blood sample. This arterial blood test will let the physician know how well your lungs are bringing in oxygen and getting rid of carbon dioxide, a waste product in the blood.
If you are ever in the hospital with breathing problems, or if your doctor thinks it is necessary as an outpatient, he/she might order a test called an arterial blood gas (ABG). This is blood test that requires the respiratory therapist to draw a small amount of blood from an artery instead of a vein like you might be familiar with. Usually, the blood sample is taken from the artery in your wrist right where you feel your pulse in thumb side of your wrist. The location can be very sensitive, so you may feel anxious before the procedure. The best practice would be for you to focus on breathing slowly in and out as they get the blood sample. This arterial blood test will let the physician know how well your lungs are bringing in oxygen and getting rid of carbon dioxide, a waste product in the blood.
Your doctor wants you to live well with COPD. Each of these tests discussed here serve a different purpose and help the doctor understand more about your lung health. The more they learn about your individual situation, the better they can help design a treatment and therapy plan that works well for you.